By Nina Mohamed
Meningitis is inflammation of the meninges, which are protective layers that surround the brain and spinal cord. It can be caused by different types of pathogens including bacteria, viruses, and in rare cases fungi. Viral meningitis is usually mild and often resolves without treatment. Bacterial meningitis is far more serious and can become life threatening very quickly. One of the serious forms is Meningitis B, caused by Neisseria meningitidis serogroup B, due to how rapidly it develops and the severity of its complications.


The bacterium responsible, known as meningococcus, was first identified in 1887 by Anton Weichselbaum. Before this discovery, outbreaks were poorly understood and often fatal. Large scale epidemics occurred in Europe and North America in the late nineteenth and early twentieth centuries, especially in crowded environments such as military camps and schools. At that time, there were no effective treatments and death rates were extremely high.
Treatment improved significantly in the twentieth century with the introduction of antibiotics. In the 1930s, sulfonamide drugs were first used, followed by penicillin in the 1940s. These drugs work by either stopping bacterial growth or killing the bacteria directly. This reduced death rates and made the disease treatable if caught early. However, Meningitis B remained difficult to manage because it can develop very quickly and lead to serious complications such as septicemia, which is blood poisoning, as well as brain damage, hearing loss, and limb loss.
Neisseria meningitidis is described as a gram negative diplococcus. This means it is made of round cells that occur in pairs, and it has a specific cell wall structure. Gram negative bacteria have a thin inner layer and an outer membrane that protects them and can make them harder to treat with certain antibiotics. The bacterium lives in the back of the throat and nose, an area called the nasopharynx. It spreads through droplets from coughing, sneezing, or close contact. Many people carry the bacteria without becoming ill, but in some cases it enters the bloodstream and reaches the brain.
To infect the brain, the bacteria must cross the blood brain barrier. This is a protective system of tightly packed cells that normally prevents harmful substances from entering the brain. Once the bacteria pass this barrier, they trigger inflammation in the meninges. Serogroup B is particularly difficult for the immune system to recognise because its outer coating is similar to molecules found in human nerve cells. This makes it harder for the body to detect it as a threat and also makes vaccine development more complex.
Early symptoms of Meningitis B are often vague and can look like common viral illnesses. These include fever, headache, vomiting, and sensitivity to light. As the disease progresses, more severe symptoms appear, including neck stiffness, confusion, seizures, and sometimes a purplish rash caused by bleeding under the skin. One of the most dangerous features of the disease is how quickly it worsens, with patients potentially becoming critically ill within hours.
Recent cases in the UK and Europe show that awareness remains important, especially among teenagers and university students who often live in close contact with others. Public health campaigns focus on recognising symptoms early and seeking urgent medical care. Although vaccines have reduced overall case numbers, outbreaks still occur.
A major breakthrough in prevention came with the development of vaccines for Meningitis B. Traditional vaccines target the outer sugar coating of bacteria, but this approach did not work well for serogroup B because of its similarity to human cells. Scientists instead used a method called reverse vaccinology, which involves analysing the genetic material of the bacterium to identify proteins on its surface that can trigger an immune response. This led to the development of the Bexsero vaccine, introduced in the UK in 2015. It has significantly reduced cases in vaccinated populations.
Treatment today involves rapid use of intravenous antibiotics, which are delivered directly into the bloodstream, along with supportive care such as fluids and oxygen. Even with treatment, recovery can be difficult and some people experience long term complications. This highlights the importance of prevention and early intervention.
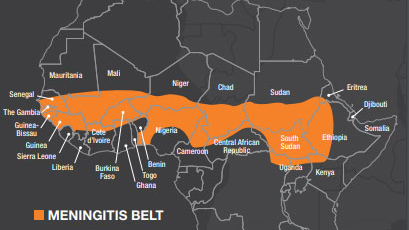
A key global case study is the region in sub Saharan Africa known as the ‘meningitis belt’. This area experiences frequent outbreaks due to factors such as climate, population density, and limited access to healthcare. Dry and dusty conditions can damage the lining of the respiratory tract, making it easier for bacteria to enter the body. Although large vaccination campaigns have reduced some types of meningitis in this region, it remains a significant public health challenge.
In summary, Meningitis B shows how infectious diseases can be both biologically complex and medically urgent. Since its identification in the nineteenth century, advances in antibiotics and vaccines have greatly improved outcomes. However, its rapid progression and potential for severe complications mean it remains a serious threat. Continued research, vaccination, and public awareness are essential in reducing its impact.
Image address, date accessed, 25/03/26:
https://www.cdc.gov/meningococcal/media/images/meningitisbelt_1.png


Add comment
Comments